This is very important to read if you have had any lymph nodes removed. Your surgeon and nurses will explain the risk of lymphoedema to you when you are in hospital for your surgery. But, as with a lot of information which is given to you right now, you may not take in what they say. So here is our top ten list of all things lymphoedema
We’ve written this article from our own experience as patients and we encourage you to speak to your medical team about your personal situation.
1. With fewer, or no, lymph nodes in your arm you are at risk of something called lymphoedema occurring in that arm. For those people who have nodes removed from both armpits, you are at risk of lymphoedema in both arms. And some people develop lymphoedema in their breasts. And you are at risk from now on. For ever. And ever. There is no cure for lymphoedema BUT the symptoms can be controlled.
2. Lymphoedema is a condition that causes your affected arm/hand/breast to swell up. We are not going to try to explain why that happens (far too technically medical for us) but if you want more information on the how’s and why’s we have listed some websites at the end of this section. You could also check out this Q&A from Natalie Kruger, Cancer, Palliative Care and Lymphoedema Physiotherapist and the Brisith Lymphology Society have an excellent fact sheet explaining lymphoedema.
3. The swelling usually happens gradually but in some cases it can come on suddenly. You should look out for signs that indicate your arm might be about to start to swell as a result of lymphoedema. According to the NHS website :
“The main symptom of lymphoedema is swelling in all or part of a limb or another part of the body. It can be difficult to fit into clothes, and jewellery and watches can feel tight.
At first, the swelling may come and go. It may get worse during the day and go down overnight. Without treatment, it will usually become more severe and persistent.
Other symptoms in an affected body part can include:
• an aching, heavy feeling
• difficulty with movement
• repeated skin infections
• hard, tight skin
• folds developing in the skin
• wart-like growths developing on the skin and/or fluid leaking through the skin”
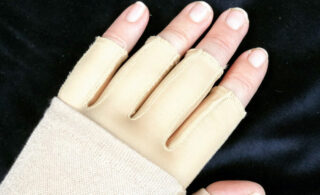
4. If you notice any of these signs, or your arm/hand/breast starts to swell, you need to seek medical assistance – call your breast care nurse, your GP or even one of the nurse helplines (Macmillan or Breast Cancer Now) who can advise you what to do. Medical treatment for lymphoedema includes draining the fluid and wearing a compression garment.
5. After breast cancer surgery it is worth taking steps in your everyday lives to avoid lymphoedema. This means avoiding infections in that arm, not over-using it and generally taking care of it. Your breast surgeon and nurses will give you some advice and the Cancer Research UK website has a good list of ways to help prevent lymphoedema. As does Breast Cancer Now. It’s important to get good advice about what you can and cannot do in life, but also to remember that being a risk from lymphoedema doesn’t necessarily mean you can’t do the things you love such as exercise and lifting weights – you just need to get the right advice from a qualified person who knows your situation.
6. If you have had the lymph nodes removed from your arm, then for the rest of your cancer treatment (and beyond) remember to not have blood tests, injections, IV and blood pressure on your bad arm. If you have had nodes removed from both arms then you can have blood pressure taken on your legs and your surgeon will tell you about having future injections in other parts of your body – not your arms. For more information about this, check out this Lymphoedema Support Network video featuring one of the leading lymphoedema specialists, Professor Peter Mortimer.
7. Consider getting a medical bracelet to wear on your arm engraved with:
Your name
Risk of lymphoedema in [R/L] arm
No BP/IV/ needles in [R/L] arm
8. Ask your GP/breast care nurse/oncologist to refer you to your local lymphoedema service who can give you more advice about the risks and what to do if you develop lymphoedema.
9. DON’T PANIC if you develop lymphoedema. It can be controlled by lymphatic drainage massage and by wearing compression garments. Manual lymphatic drainage massage is where a trained practitioner uses a very light special massage technique to help move the lymph away from areas where there are no lymph nodes (such as your arm from where your lymph nodes have been removed) to other parts of your body where you have more lymph nodes (such as your back, chest, neck or stomach). It doesn’t hurt, but because toxins are moved around your body it is important to drink lots of fluids to flush them out. Depending on the amount of swelling, you will usually have the treatment for an hour every day for a number of weeks, and then this will be gradually reduced to the point where you would only need a maintenance session every month or less. More information is available on the Macmillan website.
10. There are plenty of ways to manage your lymphoedema at home including:
• Look after your skin (to keep it silky smooth, hydrated and happy, and reduce the risk of infection)
• Exercise (see our posts from yesterday about the types of exercise you could do).
• Keep your weight under control.
• Elevate the swollen area when possible (have an ottoman under your desk at work…throw a pillow under your mattress for night elevation…pop your arm on the edge of the sofa or armrest…get creative!).
Further information
There is so much helpful information available to help you manage and cope with lymphoedema.
Further resources on our website:
Q&A with Lady Lymphoedema (aka Natalie Kruger, Cancer, Palliative Care and Lymphoedema Physiotherapist.
Article on surgical options for lymphoedema by Alex Ramsden of the Oxford Lymphoedema Practice.
Exercise can help prevent lymphoedema, by Rebecca Sellers, Physiotherapist.
Charities that provide support and information:
Make a cuppa, set aside a chunk of time and explore the websites of these wonderful charities. They have a huge amount of information, advice, videos, resources and support but you’ll need to spend some time looking through everything they offer.
British Lymphology Society – this is a professional body for members of the medical profession treating lymphoedema patients but there is also a lot of helpful information for patients on their website. You can also follow them on social media (Twitter and Instagram) for helpful updates and advice.
The Lymphoedema Support Network – this charity supports lymphoedema patients with a wealth of information and advice, as well as supporting health care professionals. You can also follow them on Twitter and Instagram for helpful updates and advice.
Where to find advice and information on the internet (focusing on UK):
Breast Cancer Now booklet on living with lymphoedema after breast cancer surgery can be downloaded or ordered here
Have a listen to the My Breast Health podcast episode 25 which covers exercise in general and how it helps lymphoedema
Lymphoedema United is a superb resource where you can find loads of information about lymphoedema management and treatment.
Breast Advocate App – this App was founded by Dr. Minas Chrysopoulo, an internationally recognized expert in breast cancer reconstruction. The App focuses around breast surgery and there is a section on lymphoedema, the aim of which is to help with your decision making processes in relation to lymphoedema.
Fact sheet from BLS on modern surgical options for lymphoedema
Fact sheet from BLS on activity and exercise
Fact sheet from BLS on what is lymphoedema
Fact sheet from BLS on simple lymph drainage
Fact sheet from BLS on what information, advice and support should be provided for those at risk of lymphoedema including the signs of lymphoedema
Lymphatic Network – a US organisation with loads of information and factsheets
Social media
Lady Lymphoedema on Twitter and Instagram – great advice and very approachable.
Lymph-what-oedema a website, practical advice, blogs, online community and follow on Twitter (@Lymphwhatodema)
@Rebeccaelwell3 – Lymphoedema clinical lead
@Lymphwales – Dr Melanie Thomas, clinical director Lymphoedema Network Wales
Finding a professional to help you:
British Lymphology Society directory of lymphoedema treatment services
To find a manual lymphatic drainage practitioner in your area, you can check out the Manual Lymphatic Drainage UK website
Videos:
The Lymphoedema Support Network library of videos on YouTube covering things like wearing compression garments, access to specialist care, how diet and exercise can help and so much more.
The British Lymphology Society have a host of videos on different aspects of lymphoedema management and treatment.
Macmillan video on compression garments.
Macmillan video on “What is lymphoedema?”
Macmillan video on treating and managing lymphoedema
Cancer Rehab PT videos on lymphatic drainage massage
The breast cancer physio has some videos about managing lymphoedema including one on Self Lymphatic Drainage Massage for Breast Cancer Related Lymphoedema
Books:
Navigating Lymphoedema: A Guide For Cancer Survivors by Teresa Lee
Let’s Talk Lymphoedema: The Essential Guide to Everything You Need to Know by Professor Peter Mortimer and Gemma Levine
Moving Through Cancer: An Exercise and Strength-Training Program for the Fight of Your Life – Empowers Patients and Caregivers in 5 Steps by Dr. Kathryn Schmitz
Future Dreams hold a range of support groups, classes, workshops and events to help you and your carers during your breast cancer diagnosis. These are held both online and in person at the London-based Future Dreams House. To see what’s on offer and to book your place, see here.
To return to the homepage of our Information Hub, click here where you can access more helpful information, practical advice, personal stories and more.
Reviewed April 2023
The information and content provided on this page has been written from a patient’s perspective then reviewed by a breast care nurse and it is intended for information and educational purposes only. It is not intended to substitute for professional medical advice. Please contact your medical team for advice on anything covered in this article and/or in relation to your personal situation. The links and/or recommendations in this article to third-party resources are for your information and we take no responsibility for the content contained in those third-party resources. Any product recommendations made in this article are not product endorsements and unless otherwise stated, they are made without any affiliation to the brand of that product. We ask you to note that there may be other similar products available.
Share

Support awareness research
Donate to those touched by BREAST cancer
Sylvie and Danielle began Future Dreams with just £100 in 2008. They believed nobody should face breast cancer alone. Their legacy lives on in Future Dreams House. We couldn’t continue to fund support services for those touched by breast cancer, raise awareness of breast cancer and promote early diagnosis and advance research into secondary breast cancer without your help. Please consider partnering with us or making a donation.



